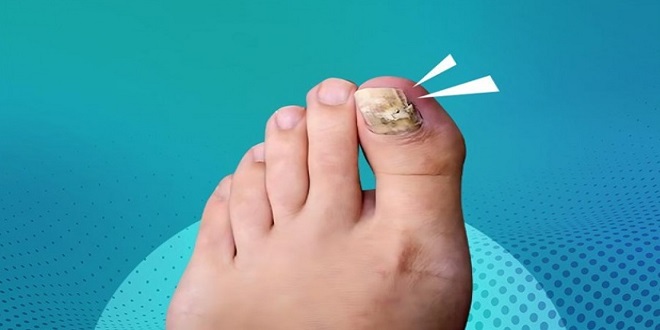
A fungal infection on nails, commonly known as onychomycosis, is a condition that affects the nails, usually the toenails or fingernails. It is caused by various types of fungi, with the most common being dermatophytes, yeasts, and molds. Fungal infections of the nails can be unsightly and uncomfortable, and if left untreated, they can lead to further complications. It can also be caused by candida.
Onychomycosis typically starts at the tip of the nail and gradually spreads to the nail bed and the surrounding areas. The infection can cause the nails to become discolored, thickened, brittle, and crumbly. They may also develop an unpleasant odor. In some cases, the nail may separate from the nail bed, a condition known as onycholysis. The affected nail may appear yellowish, white, brown, or even black, depending on the type of fungus involved.
Fungal infections on nails are more common in toenails than fingernails due to several factors. Feet are often exposed to warm, moist environments such as sweaty shoes or public swimming pools, which provide an ideal breeding ground for fungi. Additionally, reduced blood circulation in the toes compared to the fingers makes it more difficult for the body’s immune system to combat the infection effectively.
Several risk factors contribute to the development of fungal nail infections. These include:
- Age: The prevalence of onychomycosis increases with age. Older individuals are more susceptible due to slower nail growth and decreased blood circulation.
- Diabetes: People with diabetes have a higher risk of developing fungal infections as the condition affects blood circulation and weakens the immune system.
- Weakened immune system: Conditions such as HIV/AIDS or undergoing immunosuppressive therapy increase the likelihood of developing fungal infections.
- Nail trauma: Injuries to the nail, including small cuts or cracks, can create an entry point for fungi.
- Poor foot hygiene: Inadequate foot care, including not drying feet thoroughly after bathing or wearing tight-fitting shoes, can contribute to fungal growth.
If you suspect a fungal infection on your nails, it is important to seek medical advice for proper diagnosis and treatment. The diagnosis of onychomycosis may involve a physical examination, nail scraping for laboratory analysis, or in some cases, a nail biopsy.
Treatment options for fungal nail infections include topical antifungal medications, oral antifungal drugs, or a combination of both. Topical treatments are generally applied directly to the affected nails, while oral medications are prescribed for more severe cases or when topical treatments have not been effective. It is important to note that treating fungal nail infections can be a lengthy process, often taking several months to see significant improvement.
In addition to medical treatments, there are several preventive measures individuals can take to reduce the risk of fungal nail infections:
- Keep nails clean and dry: Regularly wash and dry your nails thoroughly, paying attention to the spaces between the toes.
- Practice good foot hygiene: Wear clean socks made of natural materials that absorb moisture, and change them frequently. Avoid walking barefoot in public places.
- Trim nails properly: Cut nails straight across and avoid cutting too close to the skin. Use clean, sterilized nail clippers or scissors.
- Wear breathable footwear: Choose shoes made of breathable materials that allow air circulation and reduce moisture build-up.
- Protect your feet: In public areas where fungi may be present, such as swimming pools or locker rooms, wear sandals or flip-flops to minimize direct contact with the floor.
Fungal infections on nails can be stubborn and persistent, requiring patience and consistent treatment. By following good foot hygiene practices and seeking appropriate medical care, individuals can effectively manage and prevent these infections, promoting healthy and aesthetically pleasing nails.
 Naasongs.fun
Naasongs.fun